Elderly at small residential care homes face challenges getting COVID-19 vaccine
Pictured above: Alberto Solano, a caregiver at Casa Rivera Assisted Living & Memory Care in Rodeo, Calif., receives a COVID-19 vaccine from nurse Christina Ponce on Feb. 5. (Photo by Anne Daugherty ’21)
This story appeared in the Los Angeles Times on Feb. 18, 2021
By Anne Marshall-Chalmers (’22)
California’s effort to vaccinate people in residential care homes appears to have failed to reach many small facilities that are encountering problems making appointments for their residents.
The facilities, known as board and care homes, house a maximum of six residents each, but account for nearly 6,000 of the 7,400 residential care homes whose residents have been prioritized to receive the vaccine.
The facilities, tucked into residential neighborhoods throughout the state, can house nearly 35,000 older people. Los Angeles County alone has about 1,200 board and care homes, by far the most of any county in California.
The large number of board and care homes has complicated vaccine delivery, so too have the facilities’ informal structures that set them apart from larger assisted-living facilities. Board and care homes typically have no nurses on staff and no administrative office to handle paperwork and medical records. Rather, board-and-cares are usually family owned and operated, a handful of caregivers tending to their aging residents.

Nurse Christina Ponce administers the Pfizer-BioNTech COVID-19 vaccination to Juan Rivera, a caregiver at Casa Rivera Assisted Living & Memory Care in Rodeo, Calif., on Feb. 5. (Photo by Anne Daugherty ’21)
“Some of these facilities have minimal technology tools, [but] need to register their individuals, need to be able to complete some of the administrative pieces that are required by the CDC,” said Rina Shah, vice president of pharmacy operations and services at Walgreens, during a recent Kaiser Family Foundation webinar.
Shah acknowledged that the company had hit snags when trying to arrange clinics with some residential care facilities. “If they’re not part of a large organization, sometimes it’s the coordinator that’s on site having to do a lot of those pieces, so there’s a little bit more hand-holding,” she said.
In January, as news of vaccination clinics at nursing homes and hospitals made headlines, many board and care administrators wondered when CVS or Walgreens, the pharmacies assigned by the U.S. Centers for Disease Control and Prevention to distribute the vaccine, would alert them that they were up next. But at many homes, weeks went by without any communication from the pharmacies.
“We need [the vaccine] so bad,” said Lili Xu, administrator of Rose Arbor Senior Residential Care in Contra Costa County. One of her caregivers tested positive for the coronavirus in December, and though her residents all tested negative, the experience frightened her. In mid-January, she had called both CVS and Walgreens several times to try to set up a clinic.
“Nobody can give me a direct answer,” she said.
At other board and care homes, when the phone did ring, some administrators were told they may be waiting until March for their first clinic.
Some jurisdictions, including the city of Long Beach and Santa Clara and San Mateo counties, have been forced to arrange their own mobile vaccination efforts to reach the population group. In some cases, vaccination teams have to complete the paperwork themselves before they visit, said Chelsea Velez, who oversees distribution for Choice in Aging, a nonprofit in Contra Costa County.
“Some of these places don’t have a computer, don’t have the internet,” Velez said, adding that the person Choice in Aging hired for that task is often hand-delivering printed registration and consent forms before the clinics. He’s also helping to fill them out, as many board and care facilities have residents and administrators who may not be native English speakers.
Board and care homes are for older people who need assistance with bathing, eating, medication and other daily tasks but not the round-the-clock medical care of skilled nursing facilities. They are often less expensive than residential care facilities, their larger, higher-end brethren that offer a range of amenities.
The COVID-19 vaccination problems became apparent shortly after the state-run program, which enlists facilities for the no-cost vaccinations at either Walgreens or CVS, launched in December.
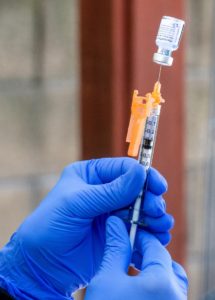
Contra Costa County nurse Christina Ponce prepares a vaccine as part of a mobile clinic run by the county and Choice in Aging, a nonprofit organization. (Photo by Anne Daugherty ’21)
Debbie Toth, chief executive of Choice in Aging, heard from frustrated board and care home owners who would call the pharmacies to get answers but were told to wait. “They say we’ll call you when we’re ready,” Toth said. “There’s nothing they can do to be proactive.”
In January, Nicole Howell, executive director for Ombudsman Services of Contra Costa, Solano and Alameda counties, received a tearful call from the owner of a facility in Alameda County who was told by CVS that a vaccination clinic wouldn’t be scheduled until March. Given that the pharmacies have had months to plan, Howell didn’t understand the delay.
“We are taking care of residents in their 90s,” said Theresa Carr, an administrator at three board and care homes in Santa Clara County. “There should have been a better plan.”
CVS has administered first doses of vaccine to 13,500 facilities, including veterans homes and retirement communities, according to its website. The pharmacy chain did not provide information on how many facilities were board and care homes.
A spokeswoman for Walgreens, Emily Delnicki, also did not provide information on the number of residents vaccinated at board and care homes. She said the chain is “on track” in vaccinating vulnerable elderly people.
In Contra Costa County, Velez, along with another administrator and two nurses make the rounds for Choice in Aging, each in their own personal vehicle to remain distanced. In one week in January, the team vaccinated about 300 residents at nearly 40 homes in Concord and Walnut Creek.
At one facility in Concord, Welcome Home Senior Residence, six residents and four caregivers sat in the living and dining rooms, some watching “Jeopardy” as the team removed vials of Pfizer’s coronavirus vaccine from a cooler. Residents were up first, rolling up their sleeves for a jab.
The mood was joyful, just as it had been at a prior location where a 96-year-old man expressed instant relief.
“I’m going to remember your name,” he told Velez. “I’m going to tell my grandchildren that you saved my life.”
Anne Marshall-Chalmers is a student in the Investigative Reporting Program at UC Berkeley’s Graduate School of Journalism. This article was written with support from The SCAN Foundation.



